- The paper presents practical guidelines for designing and managing data collection systems tailored for mobile health micro-randomized trials.
- It details methodological best practices including randomization frameworks, feature selection, and mitigation of missing data.
- Findings emphasize the importance of precise time synchronization, privacy safeguards, and robust error management in trial execution.
Practical Considerations for Data Collection and Management in Mobile Health Micro-randomized Trials
Introduction
The deployment of just-in-time adaptive interventions (JITAIs) through mobile technologies has established a paradigm shift in the design of behavioral health trials. Micro-randomized trials (MRTs) represent an experimental approach for generating data that systematically informs the sequential optimization of JITAIs by enabling randomization at a granular temporal resolution. The paper delineates practical recommendations for high-fidelity data collection and management within MRTs, drawing extensively from insights obtained in the HeartSteps physical activity study. These recommendations address feature selection, agent implementation for randomization, annotation and handling of missingness and unavailability, as well as systematized practices for robust mobile health data pipelines.
Mobile Health MRT Design: Methodological Underpinnings
MRTs diverge from standard randomized clinical trials by introducing intra-participant randomization at decision points, enabling both main and moderation effects to be examined using dense, temporally resolved data streams. The HeartSteps project exemplifies this framework, employing an Android app in conjunction with the Jawbone Up Move wearable to deliver and assess physical-activity interventions among sedentary adults.
HeartSteps randomized two intervention modalities: contextually-tailored activity suggestions delivered with probability 0.6 at each of five daily decision points, and evening activity planning randomized at probability 0.5. Both treatments targeted distinct proximal outcomes (30-minute post-suggestion step count and next-day total steps, respectively), necessitating careful temporal alignment and systematic data structuring to enable unbiased causal inference.
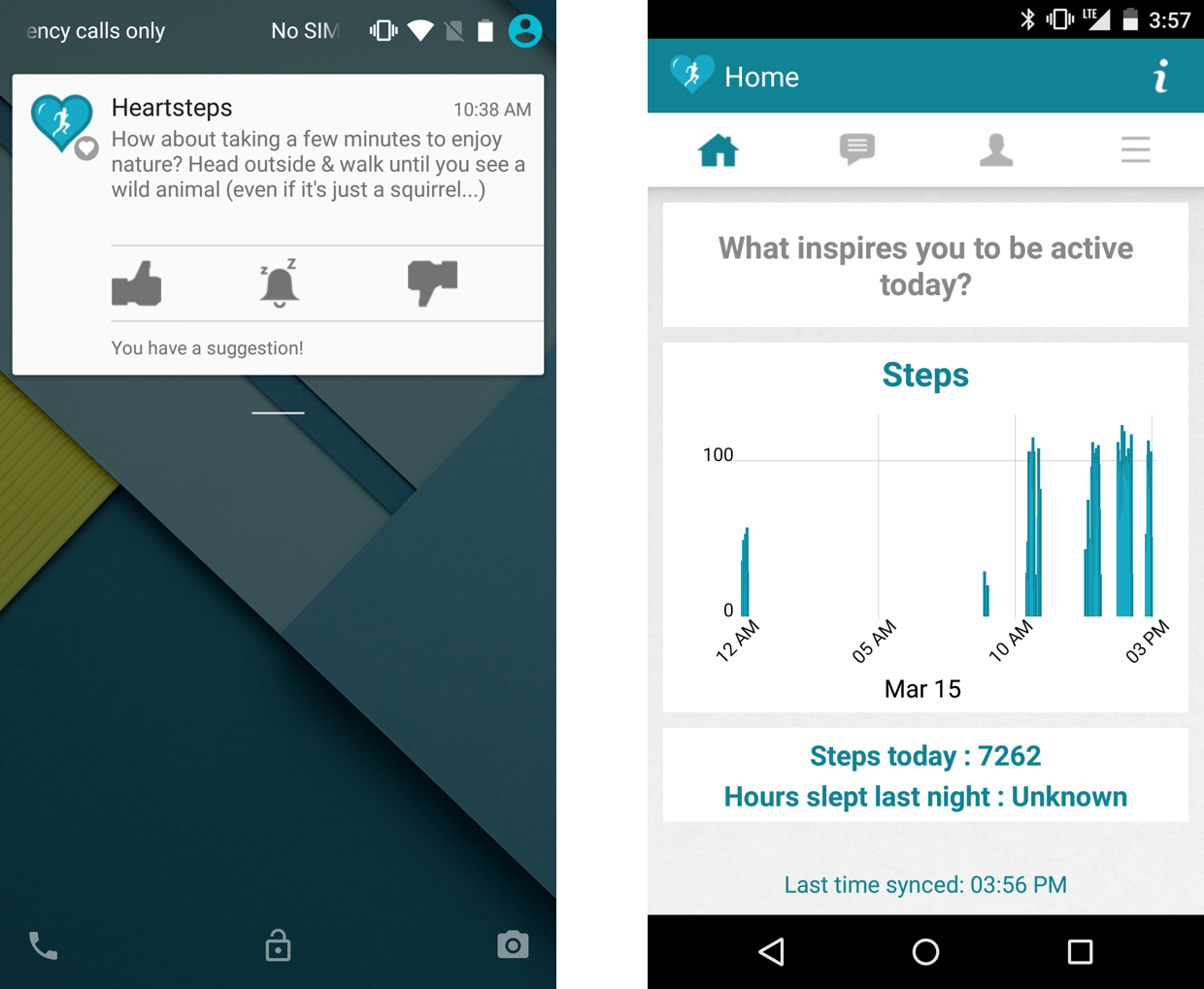
Figure 1: Screenshots of the HeartSteps app demonstrating activity suggestion delivery and participant-facing activity feedback interfaces.
Feature Selection: Causal Precision and Robustness
Determining feature acquisition protocols in MRTs must be directly responsive to scientific hypotheses centered on proximal effects. As modern smartphones and wearables offer extensive passive monitoring capabilities, restraint is essential to avoid unnecessary data collection that may compromise participant privacy or analytic tractability.
Critical to high-quality analysis is the construction of redundant proximal outcome measurement (e.g., triangulating step count with both Jawbone and Google Fit) to enable sensitivity analyses and imputation strategies robust to device- or protocol-specific missingness. Importantly, device-specific deficiencies, such as temporal granularity and sensor placement variability, must be explicitly considered to avoid confounded results.
Moderator and contextual variables are indispensable in JITAIs, as tailoring hinges on their timely and accurate acquisition. Strict protocols must be defined for collection latency; the intervention content must correspond with present context (e.g., weather, activity state) to maintain user engagement and intervention fidelity.
Randomization Agent: Architecture and Data Integrity
The architecture of the randomization agent is central to both data quality and intervention delivery latency. The trade-off between server-side and phone-side randomization encapsulates a classic tension:
- Phone-side randomization allows for minimal latency, enabling immediate, tailored intervention delivery regardless of momentary connectivity. However, it is susceptible to synchronization failures and greater risk of data loss, particularly if explicit handshake protocols between app and server are not implemented.
- Server-side randomization affords robust, centralized data logging with deterministic data structure but increases the risk of undesirable network-induced delivery delays or context misalignments. The success of either strategy demands rigorous system design and thorough pilot testing to reveal edge cases and failure states.
Missing Data and Unavailability: Annotation and Mitigation
MRTs offer a nuanced mechanism to distinguish between unavailability (protocolized exclusion from randomization due to context, such as participant driving) and genuine data missingness (from technical issues or participant disengagement). A high-quality data system must record both availability state and its determinants at each potential randomization, enabling subsequent analysis of time-varying availability patterns as a function of intervention exposure.
Explicit annotation of all missing data, with reason codes, is emphasized, especially in scenarios where device APIs or operating conditions (e.g., battery drain, sensor disconnect, user-initiated app termination) preclude data recovery. Augmenting primary sensors with redundant sources (e.g., using both Jawbone and Google Fit data streams) is an effective mitigation, facilitating imputation and sensitivity analyses.
Human and Technical Failure Modes
Mobile data collection systems are uniquely exposed to user-induced errors (e.g., disabling Bluetooth/GPS, force-closing apps) and operating-system behaviors (aggressive process management, captive portals). Proactive error trapping, frequent handshake confirmation for all data exchanges, and clear logging protocols are essential to mitigate irreparable missingness. User protocols and educational onboarding are additionally required to ensure compliance and data integrity.
Temporal Considerations and Data Synchronization
Time handling is paramount in MRTs given dense, multi-modal data acquisition and the sensitivity of causal effect estimands to precise treatment windows. The employment of UTC-based timestamps, together with local time zone tracking, minimizes ambiguity during participant travel or daylight saving transitions. The synchronization of app logs, intervention delivery, and outcome measurement hinges on meticulous timestamping and careful protocolization of feature acquisition at all relevant temporal granularities.
Privacy Preservation within Contextual Data Collection
The utility of fine-grained context data (e.g., geolocation) must be balanced against privacy risks. Appropriate aggregation (e.g., converting GPS coordinates into categorical locations such as "home/work/other") and local-only processing policies limit risk exposure. Adherence to regulatory requirements (e.g., HIPAA compliance) and judicious consideration of whether contextual features must be exported from the device form foundational privacy safeguards.
Recommendations and Implications
The paper provides a comprehensive checklist for investigators to guide system design, emphasizing a priori specification of outcomes, moderator prioritization, rigor in time handling, security and privacy safeguards, and the piloting of robust data synchronization processes. The recommendations have clear implications for future mobile health research: successful deployment of MRTs and JITAIs at scale is inextricably tied to the adoption of disciplined, transparent data engineering workflows resistant to both technical and human-induced perturbations.
As mobile interventions transition to more diverse sensors and complex adaptive designs, the need for modular, extensible data pipelines capable of integrating new data types, handling dynamic randomization probabilities, and supporting hierarchical or stratified randomization strategies will become increasingly salient. Furthermore, real-time error detection and proactive participant engagement monitoring will be essential to maintain data quality in multi-month deployments.
Conclusion
This paper operationalizes the methodological challenges in MRT data collection and management, providing systematic, empirically validated recommendations that build the foundation for scientific rigor in mobile health research. Implementation of these practices ensures that dense, context-rich data produced in these micro-randomized settings supports robust, unbiased inference on both main and moderated intervention effects, accelerating the responsible optimization of JITAIs and advancing the science of adaptive mobile interventions (1812.10800).
