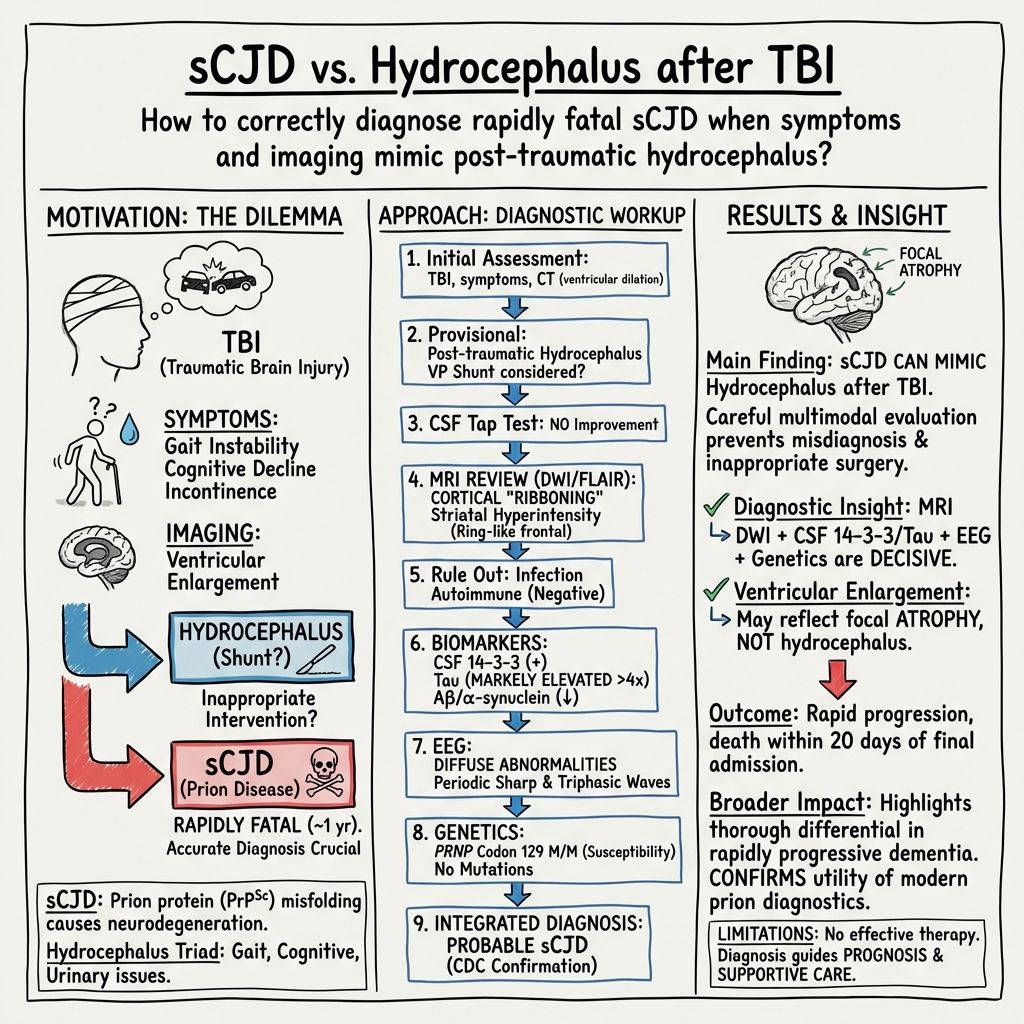
Sporadic Creutzfeldt Jakob disease presenting with cerebral atrophy following traumatic brain injury mimicking hydrocephalus a case report and literature review
Abstract: Introduction Sporadic Creutzfeldt Jakob disease sCJD is a rapidly progressive neurodegenerative disease without effective treatment that usually results in death within one year. The recently applied methods have improved the accuracy of the disease diagnosis and the specific radiological findings provide the necessary information for differential diagnosis. Research question The research is aimed to provide a different perspective on the development of CJD and associated literature review. Materials and methods The study presents a case who presented cognitive deficits, gait instability, and urinary and fecal incontinence suffered from traumatic brain injury eight months ago before admission with cerebral ventricle dilation on CT images. Furthermore, studies describe relevant cases are also included. Results The patients symptoms got deteriorated. Further examinations, including 14-3-3 and tau proteins in the cerebrospinal fluid CSF, MRI, and EEG, confirmed the patients diagnosis of sCJD. He returned to the local hospital for the conservative treatment without effective medical intervention. Conclusion This case illustrates the diagnostic process of CJD and underscores the importance of distinguishing rare disorders from common conditions to achieve a comprehensive understanding of the disease.
Paper Prompts
Sign up for free to create and run prompts on this paper using GPT-5.
Top Community Prompts
Explain it Like I'm 14
What this paper is about
This paper tells the story of a 63‑year‑old man whose brain illness looked like a common problem called hydrocephalus (too much fluid in the brain) after a head injury, but turned out to be a rare disease called sporadic Creutzfeldt‑Jakob disease (sCJD). The authors explain how they figured this out and review what other studies say about diagnosing sCJD correctly.
The main questions the authors asked
- Why did this patient’s symptoms and brain scans look like hydrocephalus at first, and how did doctors discover it was actually sCJD?
- What tests are most helpful for telling sCJD apart from more common conditions like hydrocephalus or Alzheimer’s disease?
- Could a previous head injury be related to sCJD, based on what’s known in the medical literature?
How the researchers approached it (in everyday terms)
Think of the brain like a house:
- Hydrocephalus is like a plumbing problem—too much fluid builds up, stretching the rooms (ventricles).
- Brain atrophy is like the house shrinking—walls pull inward because the structure is getting smaller.
- sCJD is like a “badly folded” building material that makes other materials fold badly too, spreading damage quickly.
This was a single, detailed case report plus a review of similar cases. Doctors used a step‑by‑step process:
- Brain imaging
- CT scan: showed enlarged fluid spaces (ventricles) that suggested hydrocephalus.
- MRI with diffusion‑weighted imaging (DWI): showed “bright ribbon‑like” signals in parts of the brain cortex—classic for sCJD and not typical for hydrocephalus.
- A “tap test”
- CSF tap test: doctors drained some spinal fluid to see if symptoms improved—this can help in hydrocephalus. It didn’t help, hinting the problem wasn’t fluid build‑up.
- Lab tests on cerebrospinal fluid (CSF)
- 14‑3‑3 protein and tau protein: These are “distress signals” released when brain cells are badly damaged. Both were high, which supports sCJD.
- Tests for infections and autoimmune diseases: negative, making those causes less likely.
- Alzheimer’s‑related proteins: some changes looked like Alzheimer’s, but the very high tau level and other clues lined up more with sCJD.
- EEG (a test of brain waves)
- Showed abnormal, periodic sharp waves—another typical sign of sCJD.
- Gene check
- A common genetic pattern in sCJD (called PRNP codon 129 MM) was present, and no inherited prion‑disease mutations were found.
Altogether, these clues pointed strongly to sCJD.
What they found and why it matters
- The patient’s symptoms (rapid memory and thinking decline, unsteady walking, trouble speaking and swallowing, incontinence) and initial CT scan looked like hydrocephalus, especially after a past head injury.
- But the MRI patterns, high 14‑3‑3 and tau proteins in CSF, EEG changes, and genetic profile all supported a diagnosis of sporadic CJD.
- Because sCJD has no effective treatment and progresses very fast, surgery for hydrocephalus (like putting in a drain called a VP shunt) would not have helped and could have added risks. Recognizing sCJD prevented an unnecessary operation.
- The patient’s condition worsened quickly, and he died about 20 days after leaving the hospital. Sadly, this rapid course is typical of sCJD.
Why it matters:
- sCJD is rare (about 1 per million people each year) but deadly, usually within a year. It can look like more common problems, especially hydrocephalus or Alzheimer’s disease.
- Using the right tests—MRI DWI “cortical ribboning,” CSF 14‑3‑3 and tau, EEG, and modern prion assays—helps doctors make the correct call sooner.
- Correct diagnosis guides care decisions, avoids unhelpful procedures, and helps families understand what to expect.
What this means for the future
- Careful, step‑by‑step diagnosis is essential when symptoms and scans are confusing. Rare illnesses like sCJD can hide behind common ones.
- There’s no proven treatment for sCJD yet. Newer lab tests (like RT‑QuIC, which can detect misfolded prion protein with high accuracy) are improving diagnosis, but cures are still needed.
- Some people developed CJD after certain medical materials used in the past (like old‑style dura grafts), but for most sCJD cases, including this one, we don’t know exactly why it starts. A prior head injury may be present in some cases, but there’s no clear proof that typical trauma causes sCJD.
- Better understanding of how misfolded proteins spread in the brain could lead to treatments that slow or stop the disease in the future.
In short: This case shows how a rare, fast‑moving brain disease can look like a more common problem after a head injury. By using the right tests and thinking broadly, doctors can reach the correct diagnosis and make the best decisions for patients and families.
Knowledge Gaps
Knowledge gaps, limitations, and open questions
Below is a focused list of what remains uncertain or unexplored in the paper and associated case, framed to guide future research.
- Lack of neuropathological confirmation: no autopsy or PrPSc typing was performed to definitively confirm sCJD and subtype (e.g., PrPSc type 1 vs 2), limiting clinico-pathologic correlation.
- Absence of RT-QuIC testing: despite discussing its high diagnostic performance, the case relied on CSF 14-3-3 and tau (which can be nonspecific post-injury), leaving unresolved whether RT-QuIC (CSF or nasal brushing) would have confirmed the diagnosis earlier and more specifically.
- Diagnostic specificity in post-TBI context: the specificity of CSF 14-3-3 and elevated tau after recent traumatic brain injury and intercurrent illness (fever, leukocytosis) was not addressed; studies are needed to quantify false-positive rates in such confounding settings.
- Imaging phenotype atypicality: the reported “ring-like” DWI hyperintensity is not standard for sCJD cortical ribboning; there is no analysis of how often ring-like patterns occur in sCJD, their differential diagnosis, or association with prior trauma—warranting systematic MRI phenotype characterization.
- Missing quantitative neuroimaging markers for NPH vs atrophy: no Evans index, callosal angle, DESH pattern, CSF flow studies, or volumetric atrophy metrics were reported; prospective validation of standardized imaging thresholds to distinguish hydrocephalus from atrophy and sCJD is needed.
- CSF tap test interpretability: the case used a tap test but did not discuss sensitivity/specificity or predictive value in differentiating hydrocephalus from mimics in the presence of neurodegeneration; controlled studies should define its diagnostic performance and failure modes.
- Multimodal imaging not leveraged: DTI, FDG-PET, or perfusion imaging were not used to refine the differential; research should test whether adding these modalities improves early discrimination of sCJD from NPH/atrophy in ventriculomegaly with gait-cognition-continence triad.
- Limited longitudinal data: no serial MRI/EEG/biomarker trajectories were presented; longitudinal profiling could clarify disease dynamics and earliest discriminative changes to prevent misdirected interventions (e.g., shunting).
- Infection control and iatrogenic risk unaddressed: the implications of performing lumbar puncture/tap tests and the initially planned VP shunt in a patient later diagnosed with sCJD were not discussed; operational studies should define biosafety protocols and risk mitigation for invasive procedures in undifferentiated rapidly progressive dementia.
- Causality between TBI and sCJD remains speculative: the paper collates prior cases but does not control for reverse causation (prodromal sCJD precipitating trauma) or confounding; population-based case–control or cohort studies are needed to test whether TBI increases risk or accelerates onset, and to characterize latency distributions.
- Co-pathology uncertainty: CSF Aβ1-42/40 reduction suggests possible AD pathology alongside elevated tau; without autopsy, the prevalence and clinical impact of AD co-pathology in sCJD—especially post-TBI—remains unresolved and merits post-mortem series and biomarker-pathology correlation.
- EEG characterization limited: EEG findings were described qualitatively without standardized metrics or evolution over time; studies should assess the incremental diagnostic value of serial EEG patterns (e.g., PSWCs emergence) in the hydrocephalus vs sCJD differential.
- Emerging biomarkers not evaluated: plasma GFAP and blood miRNA signatures (e.g., let-7i-5p, miR-16-5p, miR-93-5p) were mentioned but not tested; prospective diagnostic algorithms should quantify their incremental utility in challenging, post-TBI or hydrocephalus-mimicking presentations.
- Genetic analysis incomplete for susceptibility: only PRNP codon 129 and lack of gCJD mutations were reported; broader genomic or polygenic susceptibility profiling has not been explored to understand why some post-TBI patients develop sCJD-like syndromes.
- Clinical decision pathway not formalized: no actionable diagnostic workflow was proposed to avoid unnecessary shunting when sCJD is a possibility; development and validation of a stepwise algorithm (red flags on MRI/EEG, rapid biomarker panel, RT-QuIC) is needed.
- Therapeutic window and management unanswered: the case received only conservative care; research should test whether ultra-early diagnosis via RT-QuIC and rapid triage to investigational agents (e.g., anti-prion strategies) alters outcomes, and define best supportive regimens.
- Literature review methodology limitations: the “literature review” lacks a systematic search, inclusion criteria, and bias assessment; a formal systematic review/meta-analysis is needed to quantify the frequency, timing, imaging patterns, and outcomes of sCJD following TBI or hydrocephalus-like presentations.
- Ventricular enlargement etiology unresolved: the attribution of focal frontal horn dilation to scar-related atrophy was inferential; studies combining volumetric MRI, tractography, and (when possible) pathology are needed to validate criteria that distinguish focal atrophy from true hydrocephalus in similar cases.
Glossary
- 14-3-3 protein: A neuronal injury-associated protein used as a cerebrospinal fluid biomarker to support prion disease diagnosis. "The CSF 14-3-3 test, usually performed by western blot, has been a clinical diagnostic criterion for sCJD."
- AB1-40: A form of amyloid-beta peptide measured in CSF as part of Alzheimer’s disease biomarker panels. "The decreased proteins as AB1-42, AB1-40, and a-synuclein with the elevation of tau were the evidence of Alzheimer's disease (AD)."
- AB1-42: A form of amyloid-beta peptide measured in CSF to evaluate neurodegenerative disease. "The decreased proteins as AB1-42, AB1-40, and a-synuclein with the elevation of tau were the evidence of Alzheimer's disease (AD)."
- Akinetic mutism: A neurological state characterized by lack of speech and movement despite apparent wakefulness. "Summarizing the examination results with the typical appearances as progressive dementia, dystonia, myoclonus, psychiatric symptoms, limb tremor, cerebellar ataxia, and akinetic mutism, the patient was diagnosed with sCJD."
- Autoimmune encephalitis (AE): An inflammatory brain disorder caused by autoantibodies against neuronal antigens. "The antibody test in CSF was negative which poorly advocated the diagnosis of autoimmune encephalitis (AE)."
- Biopsy: The surgical removal of tissue for microscopic examination and definitive diagnosis. "Biopsy is mainly performed for accurate diagnosis and potential medical intervention (Watson, et al., 2021)."
- Caudate: A basal ganglia structure within the striatum implicated in motor and cognitive functions. "DWI is the most sensitive method for diagnosing sCJD, typically showing asymmetric hyperintensity in at least three cortical non-contiguous gyri ('ribboning') or the striatum (caudate and rostral putamen)."
- Cerebellar ataxia: A coordination disorder resulting from cerebellar dysfunction. "Common symptoms of sCJD include rapidly progressive dementia, cerebellar ataxia, and myoclonus (Orrú et al., 2014)."
- Cerebral atrophy: Loss of brain tissue volume due to neurodegeneration. "Cerebral atrophy and small vessel white matter ischemic changes."
- Cerebrospinal fluid (CSF): The clear fluid surrounding the brain and spinal cord, often analyzed for neurological diagnostics. "Further examinations, including 14-3-3 and tau proteins in the cerebrospinal fluid (CSF), MRI, and EEG, confirmed the patient's diagnosis of sCJD."
- Creutzfeldt-Jakob disease (CJD): A transmissible prion disease causing rapidly progressive neurodegeneration. "Among prion protein diseases, Creutzfeldt-Jakob disease (CJD) is the most common type consisting of four major groups: sporadic (sCJD), genetic (gCJD), variant (vCJD), and iatrogenic (iCJD)."
- CRP (C-reactive protein): An inflammation marker measured in blood. "The elevation of CRP and WBC indicated infectious signs."
- CSF culture: Microbiological testing of cerebrospinal fluid to detect infection. "The CSF culture result showed that there was no infectious microbe in the patient's central nervous system."
- CSF tap test: Removal of cerebrospinal fluid to assess symptom improvement, often used in hydrocephalus evaluation. "After the cognitive assessment on the 4th day, the CSF tap test was implemented to evaluate the accuracy of diagnosis and the probable efficacy after the V-P shunt."
- Diffusion tensor imaging (DTI): An MRI technique that quantifies white matter microstructure. "DTI can quantitatively assess microstructural changes in normal brain tissue (Caverzasi, et al., 2014)."
- Diffusion-weighted imaging (DWI): An MRI sequence sensitive to water diffusion, crucial for detecting sCJD-related cortical changes. "There was a wide range of ring-like hyperintense lesions in the right frontal cortex on DWI."
- Dysarthria: Impaired articulation of speech due to motor dysfunction. "Two weeks ago, he was unable to walk and exhibited dysarthria."
- Dysphagia: Difficulty swallowing, often due to neurological impairment. "The conditions deteriorated 1 week ago with the appearance of dysphagia and urinary incontinence."
- Dystonia: Involuntary muscle contractions causing repetitive movements or abnormal postures. "Summarizing the examination results with the typical appearances as progressive dementia, dystonia, myoclonus, psychiatric symptoms, limb tremor, cerebellar ataxia, and akinetic mutism, the patient was diagnosed with sCJD."
- EEG (electroencephalogram): A test that records electrical activity of the brain. "Further examinations, including 14-3-3 and tau proteins in the cerebrospinal fluid (CSF), MRI, and EEG, confirmed the patient's diagnosis of sCJD."
- Encephalomalacia: Softening of brain tissue due to injury or infarction. "Gliosis and encephalomalacia in the right fronto-temporal region, restricted diffusion throughout the cortex, most pronounced in the left parietal lobe."
- Esmolol: A short-acting beta-blocker used to control tachycardia. "The admission of esmolol to the patient relieved syndromes."
- FLAIR: An MRI sequence (Fluid-Attenuated Inversion Recovery) highlighting lesions by suppressing CSF signal. "DWI and FLAIR were recommended for diagnosis in 2009 (Watson, et al., 2021)."
- GFAP (glial fibrillary acidic protein): An astrocytic structural protein measurable in plasma as a neurodegeneration biomarker. "Plasma glial fibrillary acidic protein (pl-GFAP), associated with neuronal death, is elevated in sCJD patients (Bentivenga, et al., 2024)."
- gCJD (genetic Creutzfeldt-Jakob disease): A prion disease subtype caused by pathogenic PRNP mutations. "Among prion protein diseases, Creutzfeldt-Jakob disease (CJD) is the most common type consisting of four major groups: sporadic (sCJD), genetic (gCJD), variant (vCJD), and iatrogenic (iCJD)."
- Gliosis: Reactive change in glial cells in response to damage. "Gliosis and encephalomalacia in the right fronto-temporal region, restricted diffusion throughout the cortex, most pronounced in the left parietal lobe."
- Glycotype: The glycoform pattern of PrPSc used in molecular subtyping of prion diseases. "sCJD is classified based on codon 129 polymorphism (M and V) and PrpSe glycotype (1 and 2) into six subtypes (MM1, MM2, MV1, MV2, VV1 and VV2)."
- Homozygosity: Having two identical alleles at a genetic locus; in PRNP codon 129, associated with CJD susceptibility. "Met homozygosity at PRNP codon 129 is considered to be the most susceptible genotype for CJD, mostly in sCJD and vCJD individuals (Orrú et al., 2014)."
- Hydrocephalus: Pathological accumulation of CSF leading to ventricular enlargement and triad of gait disturbance, cognitive decline, and incontinence. "We first diagnosed the patient as hydrocephalus for the CT appearance and clinical symptoms."
- iCJD (iatrogenic Creutzfeldt-Jakob disease): CJD acquired through medical procedures or materials. "Among prion protein diseases, Creutzfeldt-Jakob disease (CJD) is the most common type consisting of four major groups: sporadic (sCJD), genetic (gCJD), variant (vCJD), and iatrogenic (iCJD)."
- Lyodura: A brand of processed dura mater graft historically associated with iatrogenic CJD transmission. "Some patients got CJD after implanting lyodura in the TBI surgery which had been reported in some cases."
- miRNA: Small non-coding RNAs that regulate gene expression and can serve as disease biomarkers. "Compared with healthy individuals, expression of three miRNAs (hsa-let-7i-5p, hsa-miR-16-5p, and hsa-miR-93-5p) is markedly decreased (Norsworthy, et al., 2020)."
- MM1: A molecular subtype of sCJD defined by PRNP codon 129 methionine homozygosity and PrPSc type 1. "sCJD is classified based on codon 129 polymorphism (M and V) and PrpSe glycotype (1 and 2) into six subtypes (MM1, MM2, MV1, MV2, VV1 and VV2)."
- MM2: A molecular subtype of sCJD with methionine homozygosity and PrPSc type 2. "sCJD is classified based on codon 129 polymorphism (M and V) and PrpSe glycotype (1 and 2) into six subtypes (MM1, MM2, MV1, MV2, VV1 and VV2)."
- MV1: A molecular subtype of sCJD with methionine/valine heterozygosity and PrPSc type 1. "sCJD is classified based on codon 129 polymorphism (M and V) and PrpSe glycotype (1 and 2) into six subtypes (MM1, MM2, MV1, MV2, VV1 and VV2)."
- MV2: A molecular subtype of sCJD with methionine/valine heterozygosity and PrPSc type 2. "sCJD is classified based on codon 129 polymorphism (M and V) and PrpSe glycotype (1 and 2) into six subtypes (MM1, MM2, MV1, MV2, VV1 and VV2)."
- Myoclonus: Sudden, brief, involuntary muscle jerks. "Common symptoms of sCJD include rapidly progressive dementia, cerebellar ataxia, and myoclonus (Orrú et al., 2014)."
- Nasal brushing: Sampling of cells from the nasal mucosa used in RT-QuIC testing for prion detection. "RT-QuIC testing of CSF has high sensitivity (80-90%), and nasal brushing from the olfactory epithelium shows 97% sensitivity and 100% specificity (Wilson et al., 2019)."
- Nasogastric tube: A tube inserted through the nose into the stomach for feeding or medication. "Due to the exacerbation of dysphagia on that day, a nasogastric tube was inserted to facilitate the provision of nutrients."
- NGS (next-generation sequencing): High-throughput sequencing used for detecting pathogens in clinical samples. "The negative result of NGS indicated that there was no infection in the patient's CSF (Dutra, et al., 2018)."
- Olfactory epithelium: Sensory tissue in the nasal cavity used for prion detection via nasal brushing. "RT-QuIC testing of CSF has high sensitivity (80-90%), and nasal brushing from the olfactory epithelium shows 97% sensitivity and 100% specificity (Wilson et al., 2019)."
- PMCA (protein misfolding cyclic amplification): An assay that amplifies minute amounts of PrPSc to improve prion detection. "PMCA requires mixing patient brain samples or CSF with normal PrPC, followed by repeated steps to reveal PrPSc in suspected samples (Bentivenga, et al., 2024)."
- PRNP: The prion protein gene; variants at codon 129 influence CJD susceptibility and subtype. "Met homozygosity at PRNP codon 129 is considered to be the most susceptible genotype for CJD, mostly in sCJD and vCJD individuals (Orrú et al., 2014)."
- PrPC: The normal, cellular isoform of prion protein. "The misfolded PrPC can cause further misfolding of normal PrPC in a cascade that results in neuronal death and associated clinical symptoms."
- PrPSc: The misfolded, disease-associated prion protein isoform. "PrPSc is the characteristic lesion of sCJD."
- PSWCs (Periodic sharp wave complexes): A characteristic EEG pattern seen in CJD. "Periodic sharp wave complexes (PSWCs) at approximately 1 cycle/second are typical CJD-like EEG findings (Puoti, et al., 2012)."
- Putamen: A basal ganglia nucleus within the striatum involved in motor control. "DWI is the most sensitive method for diagnosing sCJD, typically showing asymmetric hyperintensity in at least three cortical non-contiguous gyri ('ribboning') or the striatum (caudate and rostral putamen)."
- Restricted diffusion: An MRI finding indicating impeded water movement, often seen in acute pathology. "Gliosis and encephalomalacia in the right fronto-temporal region, restricted diffusion throughout the cortex, most pronounced in the left parietal lobe."
- Ribboning: A DWI pattern of cortical hyperintensity outlining gyri, typical of sCJD. "DWI is the most sensitive method for diagnosing sCJD, typically showing asymmetric hyperintensity in at least three cortical non-contiguous gyri ('ribboning') or the striatum (caudate and rostral putamen)."
- RT-QuIC (real-time quaking-induced conversion): A prion amplification assay used for sensitive and specific sCJD diagnosis. "Clinical application of PrPSc amplification assays, such as protein misfolding cyclic amplification (PMCA) and real-time quaking-induced conversion (RT-QuIC), has greatly improved diagnostic accuracy."
- sCJD (sporadic Creutzfeldt-Jakob disease): The most common CJD subtype with unknown cause and rapid progression. "sCJD is the predominant subtype of CJD, characterized by a median survival time of approximately one year after symptom onset (Orrú et al., 2014)."
- Striatum: A subcortical structure (caudate and putamen) involved in movement and cognition. "DWI is the most sensitive method for diagnosing sCJD, typically showing asymmetric hyperintensity in at least three cortical non-contiguous gyri ('ribboning') or the striatum (caudate and rostral putamen)."
- Tau protein (t-tau): A neuronal microtubule-associated protein elevated in CSF during neurodegeneration. "CSF t-tau is elevated in many sCJD patients."
- Tissue-based assay (TBA): An immunohistochemical test on brain tissue to detect autoantibodies in AE. "Tissue-based assay (TBA) result showed no apparent positive signal which also decreased the possibility of AE (Weller, et al., 2018)."
- Triphasic waves: A distinctive EEG waveform often associated with metabolic or prion-related encephalopathies. "EEG was abnormal for which there were significant diffuse 8 waves in the bilateral frontal and temporal lobes with periodic sharp waves, and triphasic waves in the bilateral occipital and right middle posterior temporal lobes."
- vCJD (variant Creutzfeldt-Jakob disease): A prion disease linked to bovine spongiform encephalopathy exposure. "Among prion protein diseases, Creutzfeldt-Jakob disease (CJD) is the most common type consisting of four major groups: sporadic (sCJD), genetic (gCJD), variant (vCJD), and iatrogenic (iCJD)."
- Ventriculoperitoneal shunt (VP shunt): A surgical device that drains excess CSF from the ventricles to the peritoneal cavity. "We decided to conduct a ventriculoperitoneal shunt (VP shunt) to relieve the symptoms at first."
- Western blot: A laboratory method for detecting specific proteins in a sample. "The CSF 14-3-3 test, usually performed by western blot, has been a clinical diagnostic criterion for sCJD."
- WBC (white blood cells): Immune cells measured in blood; elevation indicates possible infection. "The elevation of CRP and WBC indicated infectious signs."
Practical Applications
Immediate Applications
Below are actionable use cases that can be deployed now, derived from the case report’s diagnostic pathway and the literature it synthesizes.
- Rapid diagnostic workflow for rapidly progressive dementia (RPD) or hydrocephalus-like triads
- Sector: Healthcare (neurology, neurosurgery, emergency medicine, geriatrics)
- What: Standardize an RPD order set that prioritizes DWI/FLAIR MRI (cortical ribboning/striatum), CSF biomarkers (t‑tau, 14‑3‑3), EEG (PSWCs), autoimmune encephalitis antibody panel, CSF culture/NGS to rule out infection, and PRNP codon 129 genotyping; consider RT‑QuIC referral early.
- Tools/workflows: EHR-based order sets, diagnostic checklists, “RPD pathway” in hospitals.
- Assumptions/dependencies: Access to MRI with DWI/FLAIR, validated CSF assays, EEG availability, lab turnaround times, clinician training, referral access to RT‑QuIC-capable centers.
- “Diagnostic timeout” before ventriculoperitoneal (VP) shunt in suspected normal pressure hydrocephalus (NPH)
- Sector: Healthcare; Hospital Quality & Patient Safety
- What: Require confirmatory testing (CSF tap test, DWI/FLAIR MRI) and exclusion of sCJD before proceeding with VP shunt when imaging suggests ventriculomegaly plus gait/cognitive/continence symptoms.
- Tools/workflows: Pre-op checklist, surgical consent updates, multidisciplinary case review.
- Assumptions/dependencies: Leadership buy-in, care coordination, clinician education, appropriate scheduling windows for additional testing.
- Prion center referral and sample routing
- Sector: Healthcare delivery; Public health networks
- What: Create automatic referrals to specialized prion disease centers (for RT‑QuIC/PMCA, CDC confirmation) when RPD criteria with supportive imaging/biomarkers are met.
- Tools/workflows: Referral directories, courier logistics for CSF/nasal brushing specimens, standardized consent.
- Assumptions/dependencies: Regional availability of prion centers; specimen handling protocols; patient consent.
- Targeted adoption of nasal brushing RT‑QuIC where available
- Sector: Diagnostics; Healthcare
- What: Use olfactory epithelium brushing RT‑QuIC (high sensitivity/specificity) in patients with high clinical suspicion but equivocal CSF/imaging.
- Tools/products: Validated RT‑QuIC assays; sampling kits; biosafety protocols.
- Assumptions/dependencies: Lab capacity, regulatory status by country, training in specimen collection.
- Radiology protocol updates for suspected RPD
- Sector: Healthcare (Radiology)
- What: Ensure DWI and FLAIR are mandatory sequences for RPD; train radiologists to recognize cortical ribboning and basal ganglia involvement characteristic of sCJD.
- Tools/workflows: Protocol templates, structured reporting checklists, CME modules.
- Assumptions/dependencies: Scanner capability; radiologist education; alignment with workflow.
- Laboratory panel standardization for CSF 14‑3‑3 and t‑tau
- Sector: Diagnostics industry; Clinical labs
- What: Implement standardized, quality-controlled CSF 14‑3‑3 and t‑tau assays as part of an RPD panel; integrate reflex testing logic.
- Tools/products: IVD kits, LIS reflex rules, external quality assessment (EQA) participation.
- Assumptions/dependencies: Regulatory clearance, reimbursement, lab throughput, assay standardization.
- Systematic exclusion of mimics (infection and autoimmune encephalitis)
- Sector: Healthcare; Diagnostics
- What: Incorporate CSF culture, metagenomic NGS, and autoimmune encephalitis antibody panels early to rule out treatable causes before labeling as sCJD.
- Tools/workflows: Reflex algorithms in labs; standardized specimen volumes; interpretive comment templates.
- Assumptions/dependencies: Access to NGS/antibody testing; payer coverage; clinician familiarity.
- Infection control and surgical instrument policies for suspected prion disease
- Sector: Hospital policy; Sterile processing; OR management
- What: Enforce prion decontamination protocols (or dedicated/ single-use instruments) and biosafety procedures for suspected/confirmed cases.
- Tools/workflows: OR scheduling flags, instrument tracking, staff training, disposal protocols.
- Assumptions/dependencies: Cost and supply of single-use kits; staff compliance; updated SOPs.
- Early palliative care integration and caregiver counseling
- Sector: Healthcare; Daily life
- What: Initiate prognostic discussions, goals-of-care planning, and supportive services promptly once sCJD is suspected to avoid futile interventions and support families.
- Tools/workflows: Palliative care consult triggers; educational handouts.
- Assumptions/dependencies: Palliative care availability; clinician communication skills; cultural considerations.
- Continuing education for frontline clinicians
- Sector: Education; Healthcare
- What: CME/CPD modules highlighting sCJD presentation, key differentials from NPH/AD, and the value of DWI/CSF/EEG/RT‑QuIC.
- Tools/products: Case-based e-learning, image libraries with cortical ribboning exemplars.
- Assumptions/dependencies: Provider engagement; accreditation pathways.
- Tele-neurology/tele-radiology consultation for community hospitals
- Sector: Healthcare; Software
- What: Rapid expert review of RPD cases and MRI reads to prevent misdiagnosis and unnecessary surgeries.
- Tools/workflows: Secure image sharing, on-call expert networks.
- Assumptions/dependencies: Telehealth infrastructure; credentialing; data privacy compliance.
Long-Term Applications
These opportunities need further research, validation, scaling, or development before broad deployment.
- Multimodal AI decision support to differentiate sCJD from NPH/AD and other RPD causes
- Sector: Software; Healthcare; Diagnostics
- What: Develop models combining MRI (DWI/FLAIR), EEG, CSF biomarkers, and clinical features to assist in early, accurate triage.
- Potential products: PACS-integrated image classifiers; EHR-based risk scores.
- Assumptions/dependencies: Large, well-annotated multicenter datasets; external validation; regulatory clearance; bias and generalizability assessments.
- Point-of-care RT‑QuIC devices
- Sector: Diagnostics industry; Point-of-care testing
- What: Portable platforms for rapid PrPSc detection from CSF or nasal brushing in hospital settings.
- Potential products: Cartridge-based assays with biosafety features.
- Assumptions/dependencies: Miniaturization of assays; contamination control; CLIA/IVD approvals; cost-effectiveness.
- Blood-based triage biomarkers (e.g., plasma GFAP, miRNA signatures)
- Sector: Diagnostics; Healthcare
- What: Use pl‑GFAP and specific miRNA panels to flag probable sCJD among RPD cases before invasive testing.
- Potential products: Lab-developed tests; integrated RPD panels.
- Assumptions/dependencies: Prospective validation in diverse cohorts; clinical utility studies; cut-off standardization; reimbursement.
- Diffusion tensor imaging (DTI) and advanced MRI metrics for earlier detection
- Sector: Imaging; Academia; Diagnostics
- What: Quantitative microstructural markers to detect subclinical or early sCJD changes.
- Potential products: Automated DTI pipelines; radiology quantitative reports.
- Assumptions/dependencies: Sequence harmonization across scanners; normative databases; prospective outcome correlations.
- Therapeutics targeting misfolded prion proteins and protein degradation pathways
- Sector: Biopharma; Academia
- What: Develop and trial agents that inhibit PrPSc formation or enhance clearance (e.g., proteostasis/protein degradation approaches).
- Potential products: Small molecules, biologics, gene- or proteolysis-targeting therapies.
- Assumptions/dependencies: Translational models, BBB penetration, safety/efficacy in humans, ethical trial designs for rapidly progressive diseases.
- National RPD/sCJD surveillance and care pathways digitization
- Sector: Public health policy; Health IT
- What: Real-time reporting, registry integration, and standardized care pathways to accelerate diagnosis and ensure prion precautions.
- Potential products: Interoperable registries, automated EHR reporting triggers, laboratory–public health data bridges.
- Assumptions/dependencies: Funding, governance, privacy frameworks, interoperability standards.
- Single-use neurosurgical instrument kits for high-suspicion prion procedures
- Sector: Medical devices; Hospital supply chain
- What: Dedicated, cost-optimized disposable sets to eliminate prion contamination risk.
- Potential products: Procedure-specific kits with validated performance.
- Assumptions/dependencies: Economic feasibility, environmental impact mitigation, procurement contracts.
- Prospective studies on post-traumatic presentations and misdiagnosis reduction
- Sector: Academia; Policy
- What: Research into the intersection of TBI, ventriculomegaly, and sCJD to refine diagnostic criteria and minimize unnecessary surgeries.
- Potential outcomes: Updated guidelines; risk stratification tools for post-TBI cognitive decline.
- Assumptions/dependencies: Multicenter collaboration; standardized data capture; long-term follow-up.
- Genotype-informed diagnostics and counseling (PRNP codon 129)
- Sector: Genetics; Healthcare
- What: Use codon 129 status as a supportive diagnostic and prognostic factor; integrate into counseling for suspected sCJD.
- Potential products: Genetic testing modules within RPD panels; decision aids.
- Assumptions/dependencies: Ethical frameworks; pre/post-test counseling resources; limited utility outside diagnostic context.
- Caregiver support and digital navigation tools for ultra-rapid neurodegenerative courses
- Sector: Digital health; Daily life; Non-profits
- What: Apps and services that guide families through prognosis, infection control steps, equipment needs, and benefits navigation in compressed timelines.
- Potential products: Guided care pathways, tele-support communities.
- Assumptions/dependencies: Content validation with experts; accessibility; integration with care teams.
- Cost-effectiveness models to guide testing/management of RPD
- Sector: Health economics; Policy; Payers
- What: Economic analyses to support coverage of RT‑QuIC, CSF panels, and imaging sequences versus risks/costs of misdiagnosis and unnecessary surgery.
- Potential outcomes: Reimbursement policies; value-based care contracts.
- Assumptions/dependencies: Real-world cost and outcome data; payer engagement; model transparency.
Each application relies on local resource availability (advanced MRI, specialized labs, expert networks), regulatory environments for diagnostics, workforce training, and coordinated workflows to translate the paper’s insights into consistent practice.
Collections
Sign up for free to add this paper to one or more collections.